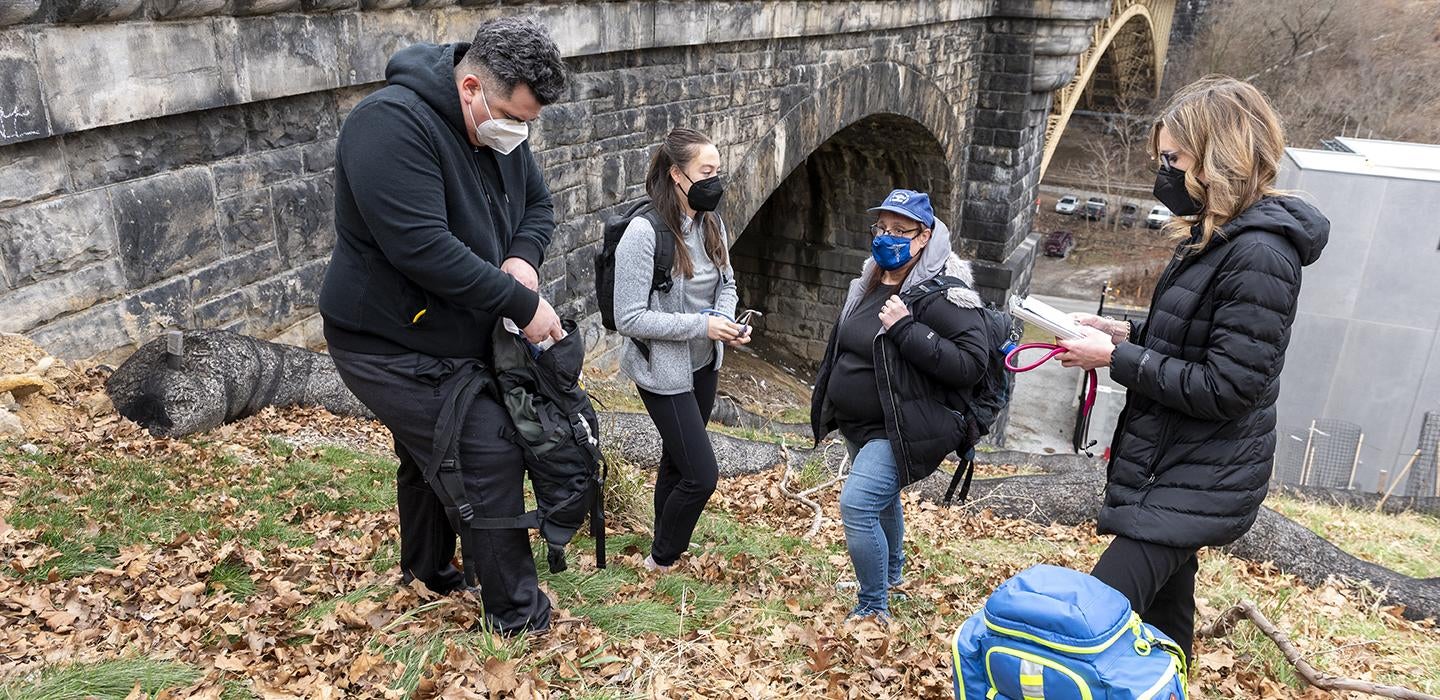Subscribe to Pittwire Today
Get the most interesting and important stories from the University of Pittsburgh.It’s a little after 6 p.m. on a Wednesday in January, and student members of Street Medicine at Pitt form a huddle on a downtown Pittsburgh sidewalk.
They’re about to start their evening rounds, providing health care, cold weather supplies and a listening ear to men who are experiencing homelessness and are waiting to enter the Winter Shelter at the Smithfield United Church of Christ.
The evening’s weather is 40 degrees with clear skies, but the temperature is expected to drop into the single digits the next day, increasing outdoor sleepers’ risks for frostbite and hypothermia.
In spring 2021, Pitt students Antonio Gumucio (MED ’19), Becky Mackenzie (ENGR ’01G), Cameron Metz and Paul Seraly (A&S ’19) created Street Medicine at Pitt to do this work — to serve Pittsburgh’s homeless population while educating future medical professionals on the realities of not having a home.
People experiencing homelessness are at a greater risk of infectious and chronic illness, poor mental health and substance abuse, according to the Center for Disease Control.
Living without a home can also impact a person’s lifespan. The average age at death of a homeless man is about 56 and the average age of death for homeless women is about 52, per an article published in PLOS One journal.
Mackenzie, a PhD student in bioengineering, and Gumucio, a Master’s of Public Health student, see Street Medicine at Pitt as an opportunity to educate their peers about the stigma that people without homes often face when seeking health care.
“We hope that club members are breaking their own stereotypes about homeless people, and students are gaining an appreciation of the cultural differences between street life and what everybody else sees,” Mackenzie said.
For Gumucio, the issue is personal. “I was in the military and unfortunately a lot of veterans end up on the street,” he said. “People who are willing to sacrifice everything shouldn’t face so many barriers to health care.”
An initiative unique to Pitt
Street Medicine at Pitt is one of only 48 student-led street medicine efforts in the world, according to Sophie Roe, chief coordinator of Street Medicine Institute Student Coalition. Pitt’s club is also the only transdisciplinary student-led street medicine effort in the country.
“We're bringing a learning community together that cuts across schools and disciplines and across degrees,” said Maureen Lichtveld, dean of the Graduate School of Public Health and one of the group’s four faculty mentors.
While only a handful of students are attending rounds on this evening, the club has over 100 members — students majoring in either undergraduate or graduate health-focused programs as varied as pharmacy, occupational therapy and public health — who participate in educational programming, including an academic journal club and guest speaker sessions.
“I’m passionate about what students are doing, and the reciprocal learning that occurs,” Litchveld said. “I help them frame their work, but I’m learning, too.”
The group’s distinguished honorary advisor, Jim Withers (MED ’84), started making “house calls” to people living on Pittsburgh’s streets almost 30 years ago, with a formerly homeless person acting as a guide and liaison.
The barriers to care Withers witnessed inspired him to start Operation Safety Net, a medical and social service outreach program for people who are experiencing homelessness in Allegheny County and the Street Medicine Institute, a non-profit that provides communities and clinicians with expert training, guidance and support to develop and grow street medicine programs. Withers is a physician at UPMC Mercy Hospital and medical director of Operation Safety Net.
Allegheny County officials estimate that there were 692 homeless people living in the county in 2021.
Step one is saying hello
Wednesday huddles start with a check-in: How is everyone feeling? Is there anyone they want to be sure to check on? What about the guy with the cough from last week? What about the folks who reside in the alley a few blocks from the shelter?
And then a supply check: Who has blankets and hand warmers to hand out? Is there anything else to distribute? Shoes? Hats and gloves?
Finally, club members pair up.
Street medicine, according to Operation Safety Net, is a patient-centered, relationship-focused and culturally sensitive care model that vows to meet and work with each patient in the context of their own reality, on their terms.
“When we serve individuals on the streets, if we do absolutely no medicine at all, it's fine,” said Anna Marie White (A&S ’02, MED ’10). She’s the medical director of Street Medicine at Pitt, a clinical assistant professor of medicine and an Operation Safety Net volunteer.
“If we get to know the person and their background, where they are coming from, then we are building trust. Meeting them where they are is what I consider a success,” she said, adding, “If we aren’t able to check their blood pressure when we see them, that’s okay, because maybe we're building towards a time whenever they will let us check it.”
By the time the students begin their rounds, 30 men are lined up outside the church’s gothic archway entrance. The shelter serves, on average, 88 people every night of operation and almost 600 individuals each year. Some appear to be the same age as the group’s youngest volunteer, a 20-year-old undergrad, and some are old enough to be her grandparent.
The students, as a way of introduction, ask the men if they need blankets or hand warmers. Then, they ask if the men have any medical needs or if there is anything the students can help them with.
One man approaches a volunteer and requests a blanket. She retrieves a few from the tote bag she’s carrying, and he unfurls and inspects each, trying to decide which to choose.
Mackenzie, one of the group's founders, advises him to pick a blanket that can best trap the air.
Mackenzie spent her teens in the late ’60s and early ’70s living on the streets of Buffalo, New York. At times, she acts as an intermediary for club members who are new to working with people who are homeless by sharing her own experience and the knowledge she’s gained by working for 30 years as a volunteer with Operation Safety Net and other organizations.
“Street life is a foreign community, in that the needs, the impulses, the motivations, the day-to-day existence — which is the preoccupation of homeless people — is not accessible by everyone else,” she said.
Building bonds
After spending two hours with shelter-goers, the club travels to central Oakland to meet a few of the people they regularly visit on street rounds who prefer to sleep outside the shelter. There is talk of hopefully convincing them to move to a shelter during the upcoming cold snap.
Student Nicole Alindogan, Street Medicine at Pitt’s operations director, said she didn’t expect to form bonds with her patients so quickly. “The relationships we build with patients are meaningful.”
Last spring, she treated a man who lived near Pitt’s campus and was reluctant at first to interact with club members. Eventually, he warmed up to the group. “He asked us about ourselves, our lives, and I learned about his life, too, even his former high school football career,” said Alindogan, who majors in pre-med and environmental studies. “He’s housed now, and I miss him. I wish we could still talk.”
Rounds end for the students as they began. In a huddle, each club member says a word that sums up their experience of the night.
Strength. Circumstances. Concern. Team. Spirit. Privilege.
— Nichole Faina