
Subscribe to Pittwire Today
Get the most interesting and important stories from the University of Pittsburgh.A new program is combating the opioid crisis while promoting better back pain management
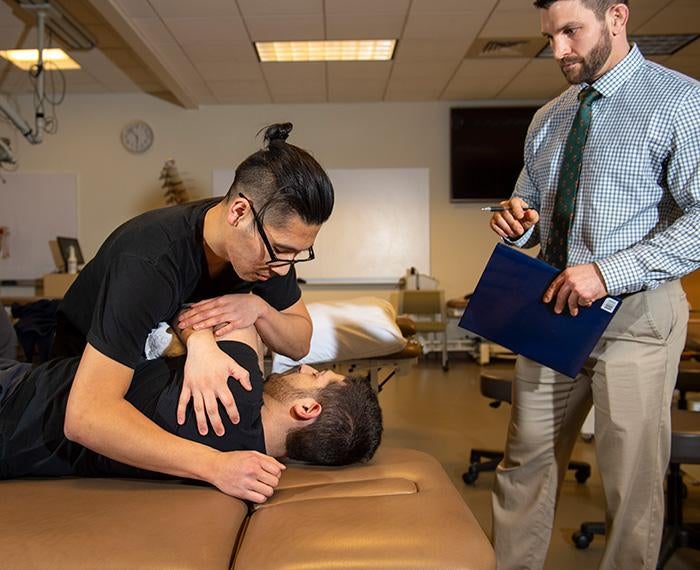
University of Pittsburgh researcher Mike Schneider has spent many years researching low back pain, including ways to treat it without performing invasive surgery or prescribing opioids.
Schneider and Pitt’s School of Health and Rehabilitation Sciences are now bringing this effort into the classroom with the Primary Spine Practitioner Certification Program, designed to train physical therapists and chiropractors to be the first-contact providers for patients with spinal problems.
Schneider and Tara Hankin, vice chair and director of the school’s post-professional education programs, said the program is unique in that it combines physical therapy and chiropractic in a multidisciplinary training program.
 “Historically, the two groups don’t play well together in the sandbox,” said Hankin. “Chiropractors have autonomous practices, and that’s well known to the public; for physical therapists, they traditionally require a referral from a physician and it isn’t obvious that they have direct-access privileges. Here, they learn from each other’s practices.”
“Historically, the two groups don’t play well together in the sandbox,” said Hankin. “Chiropractors have autonomous practices, and that’s well known to the public; for physical therapists, they traditionally require a referral from a physician and it isn’t obvious that they have direct-access privileges. Here, they learn from each other’s practices.”
“As far as we know, this is the first program of its kind,” she added.
Schneider said the program serves as an elegant, back-door solution to the opioid crisis when it comes to back pain.
“Right now, people with back pain will go to an emergency room or urgent care center and, unfortunately, a lot of them will get an opioid prescription,” said Schneider, an associate professor in the Department of Physical Therapy and the Clinical and Translational Science Institute.
Currently, about 40% of low back pain patients are prescribed opioids at some point, according to the American College of Physicians. And according to the National Institute on Drug Abuse, about a quarter of patients prescribed opioids end up misusing them. Pennsylvania experienced 5,456 drug-related overdose deaths in 2017, which represents a rate of 44 deaths per 100,000 — twice the national average. Opioids are considered the main driver of these deaths, according to the Centers for Disease Control and Prevention.
Strategies that stem opioid prescriptions when clinically appropriate could be one reason the number of opioid deaths has gone down in Pennsylvania in the past year. “If patients see a physical therapist or chiropractor, they wouldn’t be prescribed opioids because neither profession dispenses prescription medications,” Schneider said.
 “We’re hoping patients will have more confidence in the program’s graduates as first-contact providers for back pain,” Schneider said.
“We’re hoping patients will have more confidence in the program’s graduates as first-contact providers for back pain,” Schneider said.
In 2018, nearly 100 participants in the program were trained, with an accelerated cohort graduating 38 participants in April and the first traditional cohort graduating 60 students in December 2018. Another 32 students are currently registered for the second yearlong cohort, which starts in June. The total number of seats for this cohort is 60, and registration ends in May.
One graduate from the first cohort is Matthew King, a board-certified orthopedic specialist who co-owns a private practice in Irwin, Pennsylvania. King graduated from Pitt in 2007 with his Doctor of Physical Therapy degree, but returned for the PSP program.
“It was an amazing opportunity to be surrounded by physical therapy and chiropractic experts in research, clinical care and education while learning with a group of motivated professionals looking to achieve optimal patient care,” King said. “Spine care should be driven by conservative patient-centered practitioners and that is what I feel this program is aiming to achieve."
The hybrid program is divided into four units, each unit consisting of two parts: a set of online educational modules and an in person three-day skill-building workshop. Guest lecturers specializing in physical therapy and chiropractic are also brought in from across the country to teach students in the program.
Researchers want students to take with them skills to better manage patients, including eliminating unnecessary testing, decreasing opioid prescriptions and lowering treatment costs.
Schneider said the program has been about five years in the making.
“We wanted to address this huge problem in back pain management. It seems like a benign condition, but it’s one of the most mismanaged conditions and the number one cause of activity limitation worldwide,” Schneider said. “There are a lot of treatment options out there ranging from acupuncture to injections and, unfortunately, there does not seem to be a health care provider who can manage to bring order to this chaos. We want patients to be confident in choosing these physical therapists and chiropractors to manage their pain instead of looking at this uncoordinated supermarket of ideas.”

