| front |1 |2 |3 |4 |5 |6 |7 |8 |9 |10 |11 |12 |13 |14 |15 |16 |17 |18 |19 |20 |21 |22 |23 |24 |25 |26 |27 |28 |29 |30 |31 |32 |33 |34 |35 |36 |review |
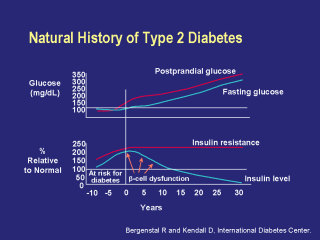 |
Before the manifestation of the metabolic
defects that lead to type 2 diabetes, fasting and postprandial insulin
levels are similar and constant. In the majority of patients in whom type 2
diabetes develops, increasing insulin resistance leads to compensatory
increases in circulating insulin, which prevents an increase in glucose
levels. As time progresses, the insulin resistance reaches a peak and stabilizes, while the compensatory increase in insulin continues to prevent fasting glucose levels from becoming abnormal. However, at some point, either because of early beta-cell dysfunction or because of a natural limit of beta-cell capacity, challenge of this delicate balance with a glucose load may demonstrate that, although fasting glucose levels remain normal, postprandial glucose levels become abnormal as a limitation in insulin response is reached. Following the onset of beta-cell dysfunction, insulin levels can no longer keep up in overcoming the insulin resistance, and fasting and postprandial glucose levels increase progressively over time. |