| front |1 |2 |3 |4 |5 |6 |7 |8 |9 |10 |11 |12 |13 |14 |15 |16 |17 |18 |19 |20 |21 |22 |23 |24 |review |
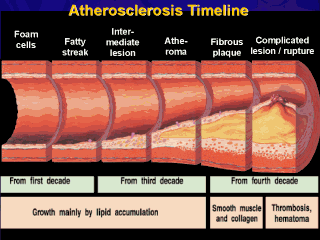 (Adapted from Pepine CJ. Am J Cardiol. 1998.) |
Atherosclerosis timeline.
Content Points:
The pathological effects of atherosclerosis occur over decades. A subtle injury to the endothelium initiates the atherosclerotic process. Endothelial dysfunction underlies many stages in the progression of atherosclerosis from earliest onset to the lesions that result in coronary heart disease (CHD). Foam cells may infiltrate the vessel, progressing to a fatty streak. As the lesion progresses, small pools of extracellular lipid form within the smooth muscle layers, disrupting the intimal lining of the vessel. Progression to an advanced lesion, or atheroma, occurs when accumulated lipid, cells, and other plaque components disrupt the arterial wall. Progression of atheroma involves accumulation of smooth muscle cells that elaborate extracellular matrix macromolecules. Once the plaque becomes fibrous, the danger of rupture increases. This type of advanced lesion can be found beginning in the fourth decade of life. The clinically important complication of atheroma usually involve thrombosis. Arterial stenoses by themselves seldom cause acute unstable angina or acute myocardial infarction. Indeed, sizable atheroma may remain silent for decades or produce only stable symptoms, such as angina, precipitated by increased demand. Thrombus formation usually occurs because of physical disruption of atherosclerotic plaque. The majority of coronary thromboses result from a rupture of the plaque’s protective fibrous cap, which permits contact between blood and the highly thrombogenic material located in the lesion’s lipid core. The endothelium participates in the atherosclerotic process and remodeling through secretion of specific compounds. These will be discussed in later slides. |